By DeVry University
March 6, 2026
6 min read
Chat with a live agent now.
No thanks
March 6, 2026
6 min read
Behind every healthcare visit is a system of medical billing and coding. Each diagnosis, procedure, and treatment relies on accurate coding to ensure providers are reimbursed properly and patients understand their portion of financial responsibilities.
If you’re considering this career field, the following medical billing and coding examples can give you a clear picture of how complex medical information is translated into standardized codes used across the healthcare system — and highlight the important role medical billers and coders play in the process.
Medical coding is the process of translating a patient’s diagnoses, procedures, and treatments from patient records into standardized medical codes used across the healthcare industry. These codes — including Current Procedural Terminology (CPT®), International Classification of Diseases (ICD), and Healthcare Common Procedure Coding System (HCPCS) — help ensure that medical information is recorded accurately, submitted correctly for billing, and easily understood by other healthcare and insurance professionals.
Medical coders need a strong grasp of medical terminology, anatomy, and healthcare regulations to assign the right codes for each procedure and diagnosis. This helps healthcare providers get reimbursed for their services and maintain accurate patient records.
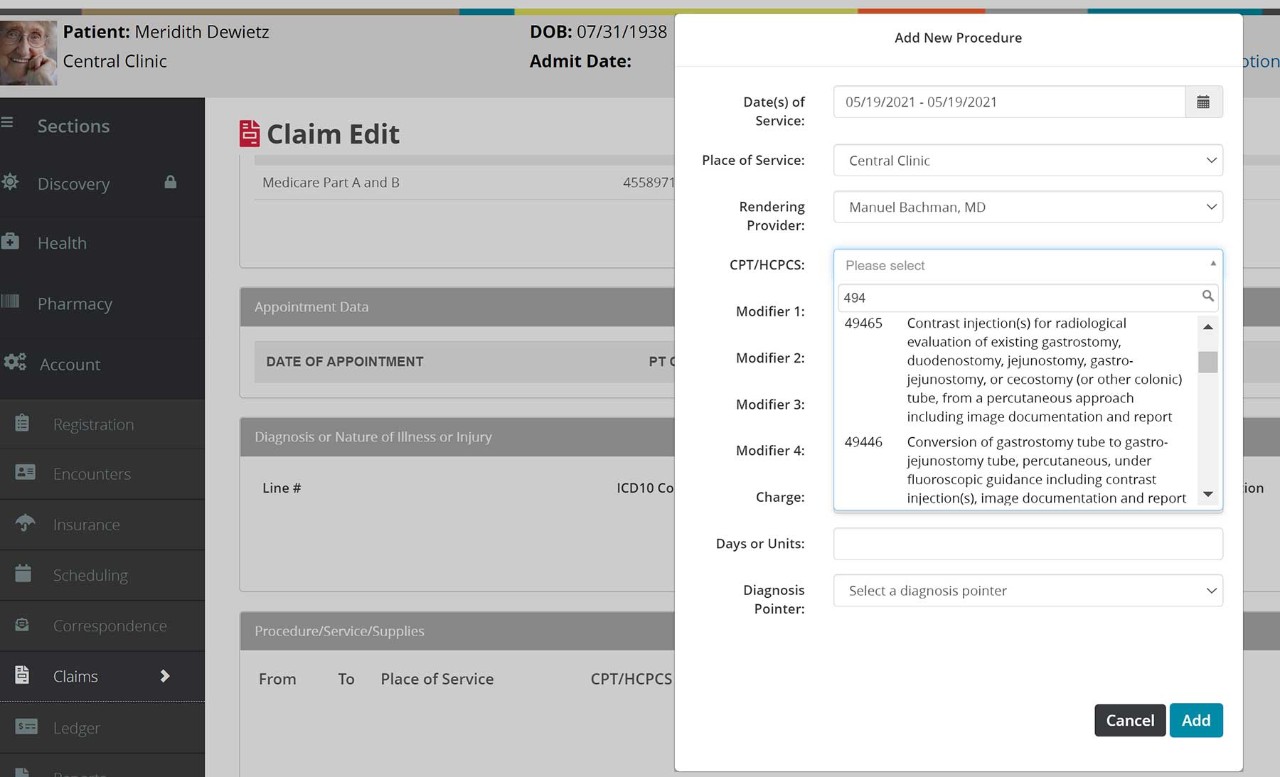
In this medical coding example, the coder receives a patient record for an abscess drainage procedure and translates the information into standardized CPT codes using the following steps:
By following this step-by-step process, the medical coder ensures that patient records are accurately represented and claims can be submitted efficiently.
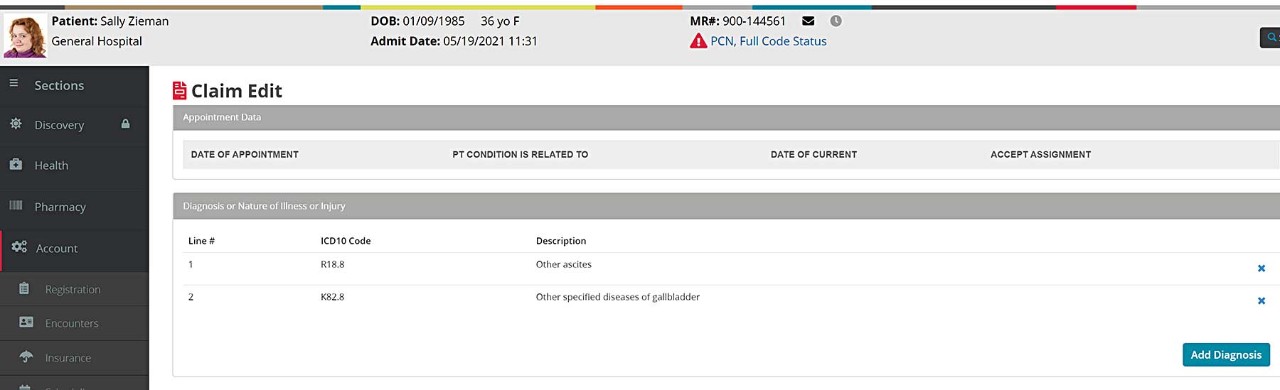
In this example, a medical coder receives a patient record for a cholecystostomy exam. Translating the details of this procedure into billing codes requires coding knowledge about ultrasound and fluoroscopic guidance in intervention radiology:
Medical billing is the process of reviewing medical records, submitting claims to insurance companies and government agencies, and billing patients for their portion. Medical billers ensure that healthcare providers are reimbursed accurately and on time, and that patients are billed for their portion of financial responsibility.
Medical billers also act as liaisons between insurance companies and patients. They track claims, resolve denials, and reprocess claims when needed, while making sure patient information is secure.
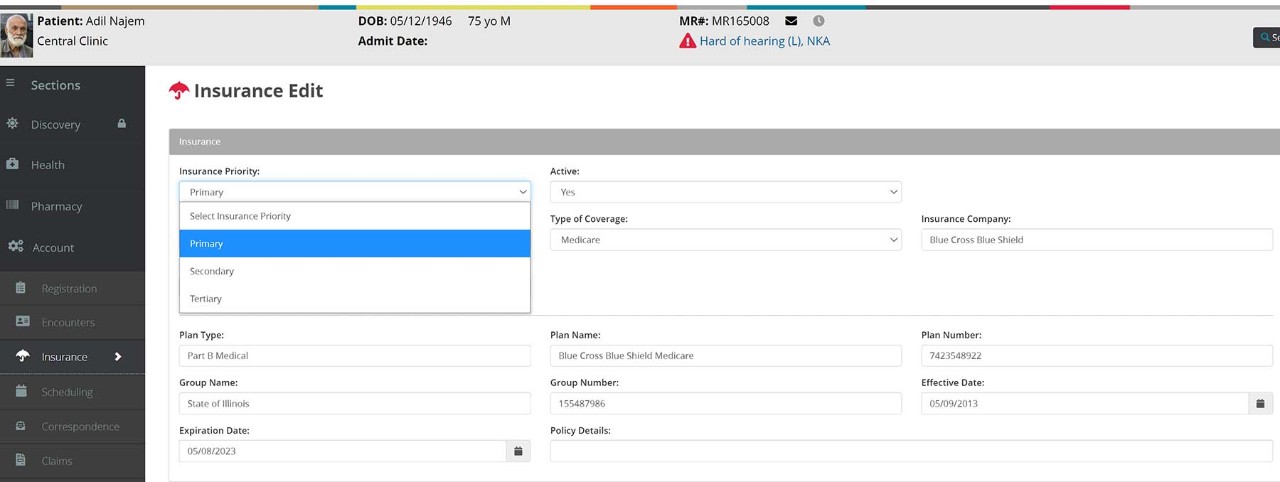
In this example, a medical biller receives a coded patient record for a cholecystostomy exam. Translating the details of this procedure for billing and submission requires coding knowledge about ultrasound and fluoroscopic guidance in intervention radiology. The medical biller uses the following steps:
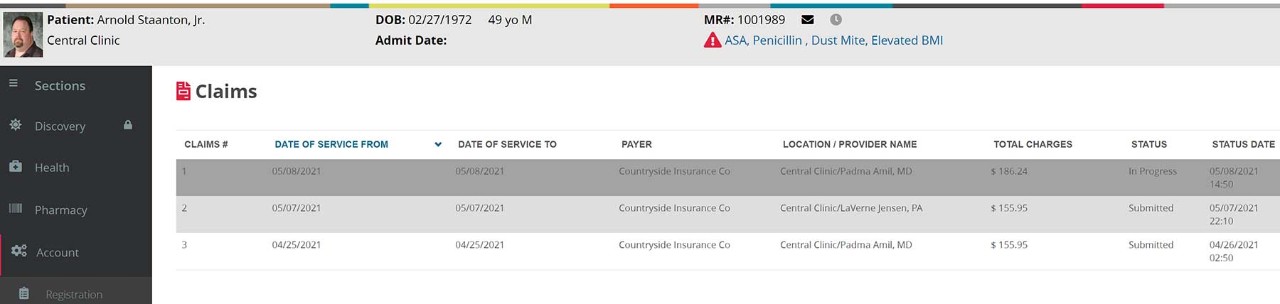
Once a procedure is completed and a medical coder turns the patient records into medical codes, the revenue cycle shifts to the back-end medical billing process. This involves creating, issuing, and managing claims until the healthcare provider is reimbursed.
Here is how a medical biller handles this part of the revenue cycle:
This behind-the-scenes work requires medical billers to be knowledgeable in health services and information systems, health information processes, and legal and regulatory issues in health information, as well as health insurance and reimbursement processes.
The information presented here is true and accurate as of the date of publication. DeVry’s programmatic offerings and their accreditations are subject to change. Please refer to the current academic catalog for details.
Ready to make an impact in healthcare behind the scenes? Your medical billing and coding career starts at DeVry.
Filter blog post category